AAAAI 2022 Highlights: Poster Presentation by FARE Educator Is Featured Among Best in Class
Congratulations to Jenna Yost and team for their research revealing food allergy management challenges among a diverse group of under-resourced individuals and families.

The annual meeting of the American Academy of Allergy, Asthma & Immunology (AAAAI) was held in Phoenix, Feb. 25-28. The hybrid in-person and virtual event included more than 150 talks and posters from FARE-supported researchers and FARE Clinical Network institutions.
FARE Health Education and Research Manager Jenna Yost (above) is the lead author on a study recently honored at AAAAI 2022. The study found that:
- The economic and psychosocial burdens associated with food allergy are high among the racially and ethnically diverse, predominantly lower-income patients and caregivers who participated in a Community Access Program survey.
- Access to emergency epinephrine is low among this group of survey participants, placing these patients at increased, avoidable risk of severe food allergy outcomes.
- Most survey participants reported food insecurity. Lacking consistent access to safe food is another factor that elevates risk of food allergy reactions and contributes to health disparities.
- Healthcare providers and advocacy groups must meet food allergy patients where they are and partner with community organizations to expand access to care, food and psychosocial support and to improve food allergy management and outcomes for at-risk populations.

With more than 600 poster presentations shared by researchers at the conference, “Improving the Understanding of Food Allergy Management and the Potential Drivers of Socioeconomic Disparities in Food Allergy Outcomes” was among the top five posters in its focus area and one of only 52 featured posters that were selected for special consideration.

Jenna’s co-authors on the study included FARE’s Vice President for Community Programs and Education Anita Roach, MS, Director of Volunteer and Community Engagement Marie Malloy, and Chief Medical Officer for Public Health Ruchi Gupta, MD, MPH, plus Justine Asante of South Ward Promise Neighborhood in Newark, N.J., and Northwestern University Feinberg School of Medicine's Isabel Galic, Ososese Enaholo, and senior study author Christopher Warren, PhD, who serves as Director of Population Health Research under the leadership of Dr. Gupta at the Center for Food Allergy and Asthma Research.

Racial, ethnic and economic disparities exist in food allergy management and care
Of the 32 million Americans living with food allergy, Black, Latinx and economically disadvantaged communities are over-represented and experience harmful food allergy-related health disparities.
- Black Americans are significantly more likely than White Americans to have food allergy.
- Black and Hispanic children are at higher risk of anaphylaxis and emergency room visits related to food allergy than White children.
- Low-income children are treated in the emergency room for food allergies around 2.5 times more often than higher-income children.
To understand these health disparities and find ways to improve food allergy care for everyone who needs it, FARE launched the Community Access Program (CAP). CAP works to promote fair and equitable access to food allergy care, management and education through programs tailored to meet the needs of the specific communities they serve across the U.S.

The Community Access Program surveyed a more diverse, less wealthy food allergy community
The CAP program research featured at AAAAI 2022 was grounded in collaboration. Clinicians, public health professionals, advocates, community partners, and survey methodologists developed the survey to assess the current food allergy management practices, attitudes and food allergy knowledge, as well as perceived barriers to quality care among low-income food allergy patients and caregivers. A community advisory board focus group was then then convened to help provide context for the data and recommend improvements.
English- and/or Spanish-speaking adult food allergy patients and caregivers were recruited through teamwork among community-based, patient advocacy, and faith-based organizations. About two thirds of participants were recruited via email or social media communications from South Ward Promise Neighborhood, an alliance of community organizations in Newark, N.J., who partnered with FARE in the CAP program’s pilot project. In July 2021, participants completed the survey online, and researchers at Northwestern University analyzed the results.
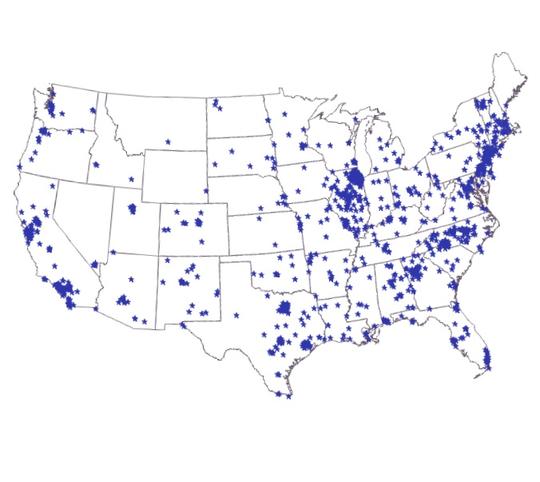
The survey was completed by nearly 6,000 participants across the nation (see map). Many belonged to groups that are typically underrepresented in food allergy research. Sixty percent were adults reporting their own food allergies, with the remaining 40 percent managing food allergies for their children or other loved ones. The majority (also 60 percent) described themselves as either non-White or Hispanic. Men and women were equally represented. Nearly all participants reported annual household income below $75,000, with 15 percent living below the federal poverty guidelines for a family of four.
The food allergies most reported by survey participants were to shellfish (28 percent), peanut (21 percent) and finned fish (18 percent). These results are largely consistent with 2019 findings that the three most common food allergies in the U.S. adult population are to shellfish, peanut and milk. Two-thirds of respondents reported having at least one food allergy diagnosed by an allergist.
Survey participants reported food allergy anxiety and lack of access to medicine and food
The CAP survey provided insight into how economic disadvantages can affect three important aspects of food allergy management
- Psychosocial impacts of food allergy
- Lack of access to the life-saving medication epinephrine
- Lack of access to safe food
Psychosocial Impacts
Among survey participants, about 30 percent of food-allergic adults reported that their food allergy caused them anxiety, and about a quarter of parents and guardians reported anxiety due to their child’s food allergy. These high levels of anxiety may reflect the degree to which low-income communities and communities of color are aware of the seriousness of food allergy: only 7 percent of survey participants, compared to about 35 percent of food-allergic individuals nationally, think there is no chance of death after accidental ingestion of a food allergen. This means that over 90 percent of those surveyed reported living with at least some degree of concern about a potentially fatal food allergic reaction.
Access to Epinephrine
About one in ten survey participants reported always having access to epinephrine, compared to about half of food-allergic individuals nationally. About 30 percent of participants had never been prescribed epinephrine, while about 12 percent received a prescription but did not fill it. The number one reason participants gave for not filling a prescription was thinking the food-allergic person did not need an epinephrine auto-injector. Educational initiatives developed in partnership with trusted community members can help raise awareness and overcome misconceptions to help food-allergic individuals stay safe.
Access to Safe Food
The availability and cost of safe food are vital issues among survey participants, who are majority non-White and below the median annual U.S. household income. More than two-thirds of participants reported using a food bank in the last 12 months, and 70 percent were at risk of food insecurity, responding “often true” or “sometimes true” to one or both of the following statements:
- Within the past 12 months, the food we bought just didn’t last, and we didn’t have money to get more.
- Within the past 12 months, we worried whether our food would run out before we got money to buy more.
Compared to participants who responded “never true” to these statements, participants at risk of food insecurity were significantly less likely to report receiving helpful food allergy resources at the time of diagnosis. These resources include written emergency action plans; epinephrine auto-injector prescriptions; epinephrine auto-injector training; information about food allergy patient organizations; information on recognizing reaction signs/symptoms; counseling on allergen avoidance; and information on interpreting food labels. Programs such as CAP can help make these valuable resources more accessible to at-risk individuals and families by helping to establish connections within their communities.
Gupta RS, Warren CM, Smith BM, Jiang J, Blumenstock JA, Davis MM, Schleimer RP, Nadeau KC. Prevalence and Severity of Food Allergies Among US Adults. JAMA Network Open 2019;2(1):e185630.doi:10.1001/jamanetworkopen.2018.5630.
Gupta RS, Warren CM, Smith BM, Blumenstock JA, Jiang J, Davis MM, Nadeau KC. The public health impact of parent reported childhood food allergies in the United States. Pediatrics. 2018 Dec 1;142(6).
Bilaver LA, Kester KM, Smith BM, Gupta RS. Socioeconomic disparities in the economic impact of childhood food allergy. Pediatrics. 2016 May 1;137(5)
2021 U.S. Federal Poverty Guidelines. Department of Health and Human Services.


